Liver Transplant
Canada
-
Our Price USD 70200
-
Hospital Price USD 78000
-
You Save : USD 7800
Booking Amount: USD 7020. Pay Remaining 90% at the hospital.
Book NowAdditional Credit
Among the important extras we offer as part of the Additional Credit are the following:
-
Site Tourism For The Patient & Attendant
-
Airport Pick & Drop Service
-
Ambulance service at airport
-
Priority appointments with The Doctor
-
Cancel Easily Anytime with Full Refund
-
Room Upgradation
-
Free Online Doctor Consultation Valued at USD 20
-
Free hotel Stay for 5 to 7 days Accordingly
-
Welcome Kit at Arrival
-
Interpreter
-
Medical Visa Assistance
What is Included?
- Doctor consultation charges
- Lab tests and diagnostic charges
- Room charges inside hospital during the procedure
- Surgeon Fee
- Cost of implant
- Nursing charges
- Hospital surgery suite charges
- Anesthesia charges
- Routine medicines and routine consumables (bandages, dressings etc.)
- Food and Beverages inside hospital stay for patient and one attendant.
What is not Included?
- Extra Radiology Investigations
- Healthcare Professionals Charges of other consultations.
- Other Requested Services such as Laundry etc.
- Additional Pharmaceutical Products and Medicines After Discharge from Hospital.
- Management of Conditions Unrelated to Procedures or Pre-Existing.
- The cost of any additional implants will be in addition to the package cost.
Package Description
Liver Transplant:
A part of a live donor's liver is surgically removed and put into a recipient's liver after the recipient's liver has been completely removed in a live donor liver transplant. The first goal of the entire procedure is to keep donors safe. When it comes to selecting and operating live donors, extreme caution is exercised.
Disease Overview:
liver cirrhosis
Cirrhosis is a late stage of liver scarring (fibrosis) induced by a variety of illnesses and disorders, including hepatitis and persistent drinking.
When your liver is wounded, whether from illness, too much alcohol, or something else, it tries to heal itself. Scar tissue arises as a result of this process. Cirrhosis causes scar tissue to grow, which makes it harder for the liver to function (decompensated cirrhosis). Cirrhosis in its advanced stages can be fatal.
Cirrhosis causes liver damage that cannot be reversed. Further damage can be reduced and, in rare cases, reversed if liver cirrhosis is discovered early and the cause is addressed.
Disease Signs and Symptoms:
Cirrhosis frequently has no symptoms until the liver has been severely damaged. When signs and symptoms do appear, they might include the following:
- Fatigue
- Bruising or bleeding easily
- Appetite loss.
- Nausea
- Legs, feet, or ankles that swell (edema)
- Loss of weight
- Skin that is itchy
- Skin and eye discolouration are yellow (jaundice)
- Your abdomen is bloated with fluid (ascites)
- Your skin has spider-like blood vessels.
- The palms of the hands are red.
- Absent or missed periods that aren't connected to menopause in women; sex drive decrease, breast growth (gynecomastia), or testicular atrophy in males.
- Drowsiness, confusion, and slurred speech (hepatic encephalopathy)
Disease Causes:
Cirrhosis can be caused by a variety of diseases and conditions that damage the liver.
The following are some of the reasons:
- Abuse of alcohol for a long time
- Hepatitis caused by a virus that has been present for a long time (hepatitis B, C and D)
- The accumulation of fat in the liver (nonalcoholic fatty liver disease)
- The accumulation of iron in the body (hemochromatosis)
- Cystic fibrosis is a disease that affects the lungs.
- Wilson's illness is a condition in which copper accumulates in the liver.
- Bile ducts that aren't properly developed (biliary atresia)
- Alpha-1 antitrypsin deficiency is a condition in which the body lacks the enzyme alpha-1 antitryp
- Sugar metabolism diseases that are passed down via the generations (galactosemia or glycogen storage disease)
- A digestive problem caused by a genetic mutation (Alagille syndrome)
- The immune system of your body causes liver disease (autoimmune hepatitis)
- The bile ducts are destroyed (primary biliary cirrhosis)
- Bile duct scarring and hardening (primary sclerosing cholangitis)
- Infections like syphilis and brucellosis are common.
- Methotrexate or isoniazid are two examples of medications.
Factors that are at risk
- Overindulging in alcoholic beverages. Cirrhosis is linked to excessive alcohol intake.
- Being overweight is a problem. Obesity raises the risk of nonalcoholic fatty liver disease and nonalcoholic steatohepatitis, both of which can develop to cirrhosis.
- Hepatitis caused by a virus. Cirrhosis does not develop in everyone with chronic hepatitis, although it is one of the most common causes of liver disease worldwide.
Disease Diagnosis:
Cirrhosis of the liver in its early stages is frequently asymptomatic. Cirrhosis is frequently discovered during a regular blood test or checkup. A combination of laboratory and imaging tests is frequently performed to assist confirm a diagnosis.
Tests Your doctor may request one or more tests to see if you have a liver disease, such as:
Tests in the lab Blood tests may be ordered by your doctor to look for indicators of liver disease, such as high bilirubin levels, as well as specific enzymes that signal liver damage. Creatinine levels in your blood are measured to determine renal function. Hepatitis viruses will be tested on you. Your blood's capacity to clot is also tested using an international normalised ratio (INR).
Your doctor may be able to determine the underlying cause of cirrhosis based on the findings of the blood tests. He or she may also conduct blood tests to determine the severity of your cirrhosis.
Imaging tests are performed. MRE (magnetic resonance elastography) may be suggested. The liver hardening or stiffening is detected with this noninvasive advanced imaging technique. Other imaging tests, such as an MRI, CT scan, or ultrasound, may be performed as well.
Biopsy. For diagnosis, a tissue sample (biopsy) is not always required. Your doctor, on the other hand, may utilise it to determine the severity, extent, and source of liver damage.
If you have cirrhosis, your doctor will most likely recommend routine diagnostic tests to check for signs of disease progression or complications, particularly esophageal varices and liver cancer.
Disease Treatment:
Cirrhosis treatment is determined by the cause and severity of your liver damage. The treatment's aims are to decrease the growth of scar tissue in the liver, as well as to prevent or treat cirrhosis symptoms and consequences. If you have serious liver damage, you may need to be admitted to the hospital.
Cirrhosis treatment for the underlying cause
It may be feasible to reduce liver damage in early cirrhosis by addressing the underlying cause. Among the possibilities are:
An alcohol addiction treatment programme. Cirrhosis induced by excessive alcohol use should be avoided at all costs. If quitting drinking is tough, your doctor may suggest an alcohol addiction treatment programme. It is vital to stop drinking if you have cirrhosis since any amount of alcohol is hazardous to the liver.
Loss of weight. Cirrhosis caused by nonalcoholic fatty liver disease can be improved if the patient loses weight and keeps their blood sugar under control.
Hepatitis treatment medications. Through particular therapy of these viruses, medications may reduce additional damage to liver cells caused by hepatitis B or C.
Medications to treat cirrhosis's additional causes and symptoms. Certain kinds of liver cirrhosis can be slowed down with medication. Medication, for example, may greatly slow the course of primary biliary cirrhosis in those who are detected early.
Other drugs can help with itching, exhaustion, and discomfort, among other things. To combat malnutrition caused by cirrhosis and to avoid weak bones, nutritional supplements may be provided (osteoporosis).
Cirrhosis consequences are treated.
Your doctor will seek to address any cirrhosis consequences, such as:
You have too much fluid in your body. Controlling ascites and edoema may be easier with a low-sodium diet and medicines to prevent fluid accumulation in the body. Fluid accumulation that is more severe may necessitate draining techniques or surgery to relieve pressure.
Hypertension in the portal veins. Certain blood pressure drugs can help avoid serious bleeding by lowering the pressure in the veins that supply the liver (portal hypertension). At regular intervals, your doctor will do an upper endoscopy to check for swollen veins in the oesophagus or stomach (varices) that might bleed.
If you get varices, you'll almost certainly require medicine to prevent bleeding. If the varices are bleeding or are likely to haemorrhage, a procedure (band ligation) may be required to halt the bleeding or limit the risk of additional bleeding. A tiny tube — a transjugular intrahepatic portosystemic shunt — may be inserted in your vein to lower blood pressure in your liver in extreme situations.
Infections. Infections may be treated with antibiotics or other medicines. Vaccinations for influenza, pneumonia, and hepatitis are also likely to be recommended by your doctor.
Increased risk of liver cancer. Periodic blood tests and ultrasound scans to check for symptoms of liver cancer will most likely be recommended by your doctor.
Hepatic encephalopathy is a kind of encephalopathy caused by liver disease. To assist lessen the accumulation of toxins in your blood owing to impaired liver function, you may be offered medicines.
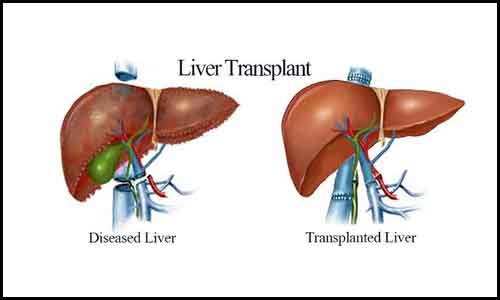
Transplantation of the liver
When the liver fails to function in severe forms of cirrhosis, a liver transplant may be the sole choice for therapy. A liver transplant is a process in which your liver is replaced with a healthy liver from a deceased donor or a portion of a living donor's liver.
One of the most prevalent causes for a liver transplant is cirrhosis. Candidates for a liver transplant go through a series of tests to see if they are healthy enough to undergo a successful surgery.
Those with alcoholic cirrhosis have traditionally been barred from receiving a liver transplant due to the danger of relapsing into hazardous drinking following the procedure. Recent research, on the other hand, suggests that people with severe alcoholic cirrhosis have post-transplant survival rates comparable to those of liver transplant recipients with other types of liver disease.
Information related to Treatment
Package Details
Days in Hospital
14 Days
Days in Hotel
*
60 Days
Room Type
Private

Treating Doctor
Dr. Mar Miserachs
Gastroenterologist- Gastrointestinal surgery, Gastro Intestinal Surgeon, Liver Cancer Treatment, Gastro Surgeon, Diabetes Specialist, Liver Specialist, Fatty Liver Specialist, Liver Transplant Specialist, Liver Diseases, Pediatric Liver Transplant
North York General Hospital Toronto, Canada
18 Years of Experience
Similar Packages
Frequently Asked Questions
In Canada, the long-term success rate of transplantation for both adults and children is more than 80%. Following are some of the top rated hospitals for Liver Transplant in Canada: 1-Toronto General Hospital (TGH) 2-Ajmera Transplant Centre
In Canada, the price of a liver transplant varies from $33,000 to $48,000.
After surgery, the majority of patients resume a good quality of life after three to six months. Anti-rejection drugs are required to be taken by all liver transplant recipients for the remainder of their lives. These are checked to make sure the patient's blood contains the appropriate dosage of medication.
The living donation procedure is a significant surgery that necessitates a two- to three-month recuperation period and a hospital stay of five to ten days. The risk of death from the donor operation is extremely minimal. The donor's liver regenerates to about 90% of its initial size in a matter of months.